Hospital to Home (H2H) brings together expert staff from across health and social care. We work together to transform how people transition from hospital to home.
We aim to start planning each person’s discharge as soon as we admit them to hospital. It’s a team effort that provides support to each patient and their family, friends, and carers.
We work together to ‘unblock’ things that are getting in the way of them getting home safely and quickly.
What does Hospital to Home do differently?
Before Hospital to Home, people’s progress through their hospital stay (known as ‘flow’) was often fragmented. Different roles, teams and organisations didn’t always work closely together.
This new team brings together experts from health, social care, and the voluntary sector into local hubs. We are working together to break down silos.
We hold daily ‘flow’ meetings, ward reviews, and virtual ‘H2H Hubs’ where we can support other teams.
Our work often involves coordinating practical solutions to problems like housing or benefits. Depending on what someone needs, we can signpost to other services or provide support ourselves. We focus on person-centered care built around each person’s rights and needs.
Working together also helps to ensure clear communication between patients, families, and professionals.
This service operates across North Cumbria and Tyne and Wear. We take the same joined-up approach wherever people live in our region.
The Hospital to Home team
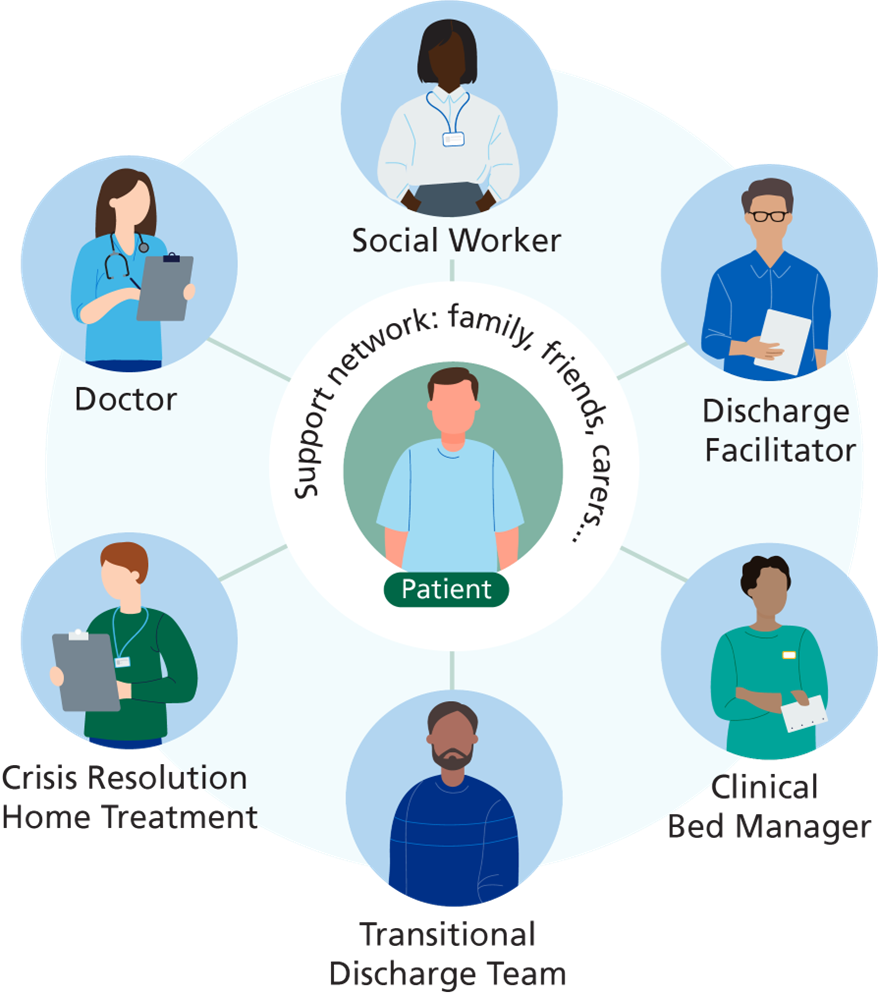
The Hospital to Home team consists of many specialist staff who all work together around the patient. Here are some of the key roles that we have within the team:
Discharge Facilitators assess, coordinate, and help people to transition to our Crisis team when they are clinically ready. They use their wealth of local knowledge and networks to support discharges.
Clinical Bed Managers in each area coordinate bed availability across the Trust. This includes giving extra help for complex or high-risk cases when someone is ready to be discharged. They also provide clinical oversight when we transfer or move people to a different level of care.
The Transitional Discharge Team helps reduce delays by identifying and fixing issues that could block someone’s discharge early on. This can mean providing practical help or directing someone to additional support. They use a network of community contacts and resources. They play a key role in making sure that discharge planning is person-centered and begins early in the admission process.
Social Workers provide leadership and legal expertise. They are especially important in interfacing between services and organisations in more complex cases. They can also do social work assessments to ensure a safe and sustainable discharge.
Senior Crisis Clinicians are skilled practitioners. They can expertly assess risks and make clinical decisions. They are the key points of contact for patients, carers and colleagues. By offering quick assessments and short‑term therapeutic input in a crisis, they can help to resolve issues before they get worse. Senior clinical oversight supports safe discharges, step-ups and transfers.
Senior Medical Consultants are skilled psychiatrists. They offer a wide range of clinical advice. They advise on complex cases, like when someone has several hospital stays or is in a ward for a long time without getting better.
Improving discharge rates and patient experience
By changing our approach, we can now send more people home from hospital when they are ready. From June to September 2025, facilitated discharges increased from 289 to 367 compared to the previous year. We were able to make 75 more discharges than the year before. This means fewer people are ‘stuck’ in hospital when they are clinically ready for discharge.
This saves money and makes sure beds are free for those who need them. Most importantly, patients say they have a better experience. Patients and their families have given us positive feedback. They appreciate when services work closely together. They also value consistent support from social workers.